The Rise of Anesthesia, 1800-1920
Today, most medical procedures are designed to be as painless as possible for the patient. But this was not the case before October 16, 1846. “Ether Day” commemorated William Thomas Green’s use of an inhaled anesthetic in a dental surgical procedure.
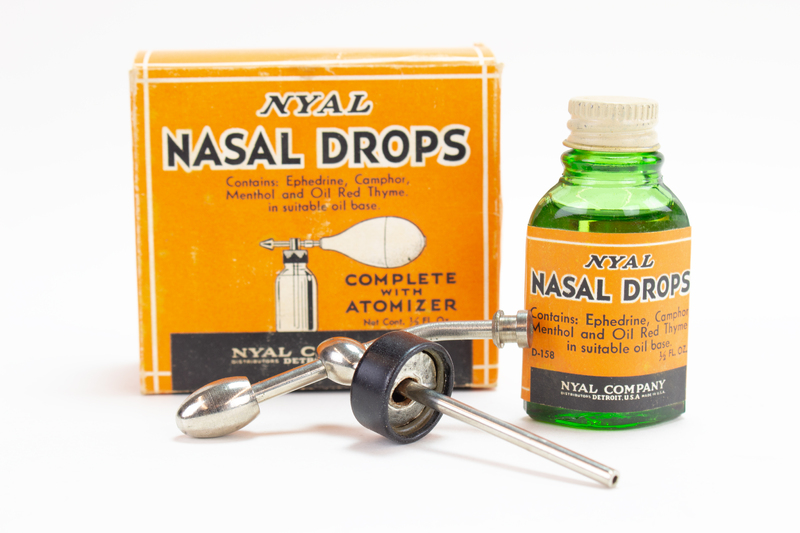
Ether, or “sweet oil of vitriol,” was first synthesized by Valerius Cordus in 1540. Joseph Priestley discovered nitrous oxide or “laughing gas” in 1772 and its use in surgery was first suggested as early as 1800. However, these compounds were primarily used for entertainment or recreational purposes until the 1840s, when both were used in dental procedures. The goal was to relieve pain and help patients recover quickly from the effects of the compounds.
After Louis Pasteur brought forth his “germ theory” in 1865 and antisepsis became routine, more complex and lengthy surgeries began to be performed. These developments required changes to inhaled anesthetic procedures and compounds.